When the pandemic spread through the United States, it did more that create a care crisis for so many healthcare organizations. It created an existential crisis, one that left healthcare administrators questioning how their organizations were put in the position as well as how were they going to bounce back.
The stewing of those questions wasn’t limited to organizations providing care, as well. It reached those who designed the facilities and campuses for care. As non-emergent services were curtailed or suspended for various reasons that affected operations and finances, the situation caused by the pandemic sparked a conversation that was both reflective and forward-thinking.
“The pandemic really unearthed or exposed us in a way that said, ‘We’ve got to be thinking about this bigger and broader. We’ve got to look at it from more lenses than just normal,’” said David Voller, ACHE, MBA, a senior operational planner at BWBR. “Because, unfortunately, we did paint ourselves into corners, whether that was limiting the number of accesses into physical space, or how we created that flow through space, limiting the amount of storage because we went to just-in-time inventory systems, or how we defined staff to have them work as optimally as possible.”
With master plans historically guiding the development of hospitals and healthcare campuses, the discussions that emanated from this examination spawned a new approach to planning. More than looking at the delivery of services occurring in the facilities, a team of design professionals examined what it would take for organizations to be able to absorb the disruptions caused by adverse events like a pandemic. Scenario planning emerged, and it’s what Voller addressed with Sophia Skemp, AIA, EDAC, and Mike Boldenow, a medical planner and principal, respectively, at the firm, in the latest episode of Side of Design.
“So that was really the genesis, planning for the unpredictable,” Skemp said. “Scenario planning is trying, as much as possible, to prevent health systems from experiencing the ramifications that they went through in 2020 and are continuing to go through today.”
Stressing that scenario planning addresses more than the financial impact that an organization incurs when events like natural disasters, pandemics, mass casualty, or facility threats occur, Skemp outlined other impacts ranging from the experience of care to care access and staff resiliency as key factors influencing the thinking behind scenario planning.
“Yes, it’s about cost, but it’s also about people, their experience of care, the health of your community, and what can we do as designers to make those more resilient,” Skemp said.
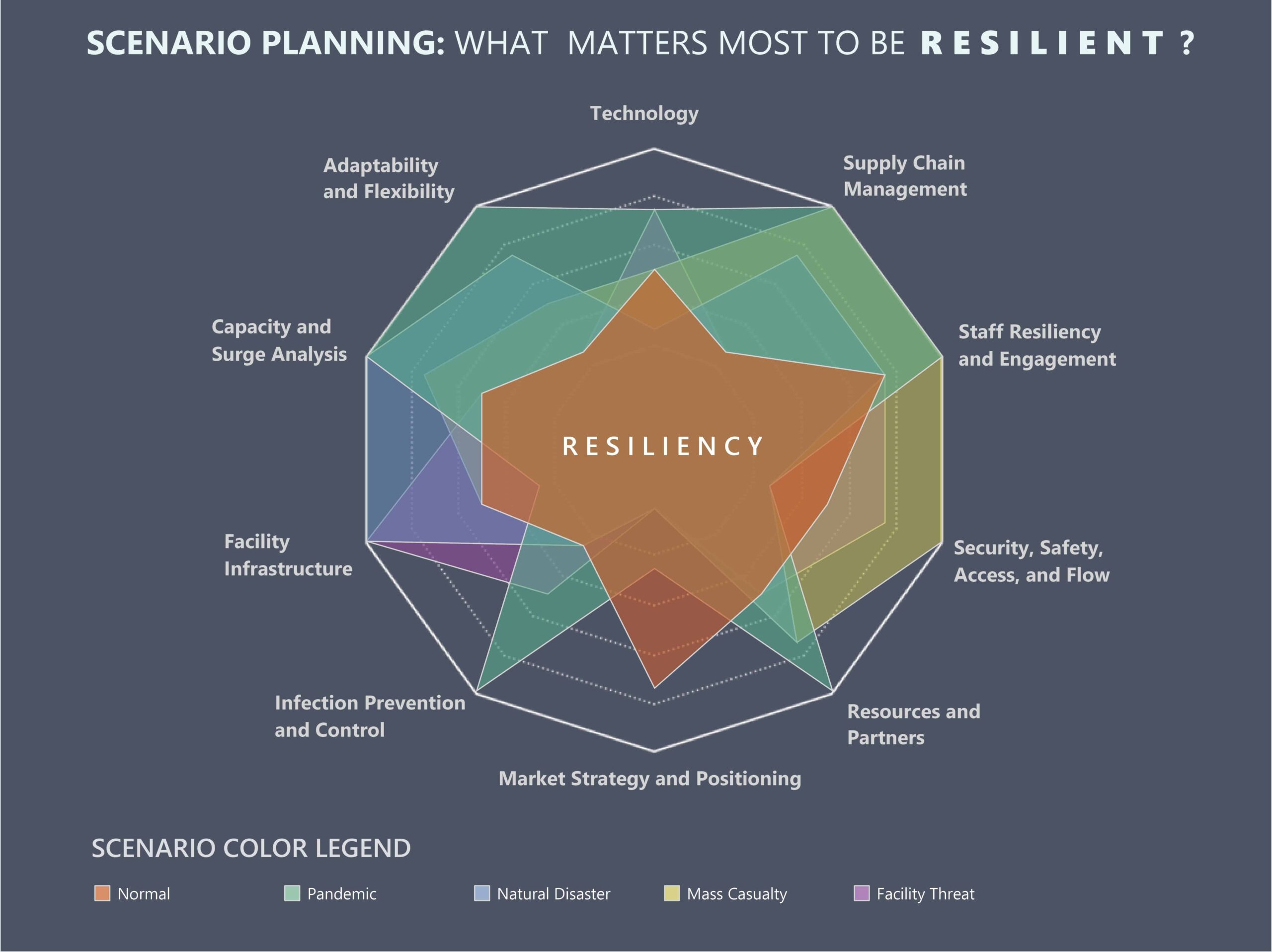
Contrasting scenario planning with the traditional master planning process, Boldenow described the two in connected terms rather than exclusive ones.
“What scenario planning is doing is evolving the process,” he said. “We’re evolving it to include information, to gather information, to ask questions that help our clients and systems prepare for those disruptions that we don’t know will ever happen. We’re not planning for another pandemic, although what we’ve learned can be applied to helping us be more resilient, whether it’s a mass casualty event, a facility threat, a natural disaster.
“We’re trying to alleviate the fear of the unknown and move forward confidently with solutions that are really going to be more operational solutions than they are physical or infrastructure-based solutions.”
“So master planning, like [Mike] said, is designing for where you are headed, based on data volumes or where you want to head,” Skemp said. “Scenario planning is helping to make sure that that is still possible, in addition to maintaining your baseline operations. So just helping the typical master plan along the way, that it’s resilient in the face of a tornado. The next COVID, for example.”
Resilient was a word that permeated much of the conversation, looking at the resiliency of operations, the resiliency of staff, and the resiliency of a facility. Applying that lens of resiliency to an organization’s operations, Voller said it allows administrators and managers from across the spectrum of the organization, such as facilities, med-surg, environmental services, and IT, to evaluate how they can respond to deviations from normal operations without putting the integrity of the organization at risk.
“I like the way scenario planning is going to shape a broader perspective. It’s a more holistic look at how we need to be prepared for running our operations and become more flexible, become more adaptable,” he said.
“It’s being able to recover and maintain form while under pressure,” Skemp said. “So, how can your facility maintain operations while under the external pressure of a pandemic, a severe weather event, mass casualty? It’s resilience. It’s the definition that’s at the heart of scenario planning.”
[Scenario planning’s] really an operational solution. We’re not trying to design bigger hospitals with more beds, in the chance that there might be a mass casualty event, or another pandemic. We’re trying to either design new facilities or adapt existing facilities just for that purpose to be flexible.
Mike Boldenow, principal
With the focus on how organizations can be resilient, however those individual organizations define that word, Boldenow said it changes the nature of the conversation, one where space is the tool that adapts to the situation to enable staff and organizations to deliver care through the variable scenarios. From private patient rooms that can be utilized for multiple patients to traffic flows that can be altered to protect non-infectious patients, scenario planning can identify those opportunities to create an operational program that flexes with the need.
“We tried to lean ourselves or our designs to meet a demand to lower healthcare costs, and that had to deal with reducing space and trying to be more efficient, which is good. Don’t get me wrong,” he critiqued. “We weren’t focused on the big picture, and, the big picture again, was the fear of the unknown. We don’t know what we don’t know.
“But now that we’ve gone through something like this, I think it’s helping us to open our eyes a little bit. This isn’t really a bricks and mortar solution, what we’re talking about here. It’s really an operational solution. We’re not trying to design bigger hospitals with more beds, in the chance that there might be a mass casualty event, or another pandemic. We’re trying to either design new facilities or adapt existing facilities just for that purpose to be flexible.”
“The pandemic was a good reminder that we need to be thinking more holistically, and we have to not lose sight of all these variables that can enter into the equation,” Voller said. “We want to think about how do we keep from getting into a scenario that [causes hospitals] to shut down operations, that puts staff in a position of being and feeling burnt out; that puts the community at additional harm’s way because we haven’t thought about how they operate in that physical space.”
Sophia Skemp, Mike Boldenow, and David Voller co-authored a white paper with Scott Holmes, RA, ACHA, LEED AP, on the approach to and benefits of scenario planning. Click to read, “Scenario Planning: How to be Resilient in Design and Operations.”