The United States has some of the highest costs of healthcare in the world, and those numbers are only going up. Margins for hospital systems are razor thin, and organizations face increasing shortages of healthcare providers in the face of burnout and challenging working conditions. And that’s before we talk about the barriers to care many patients face, whether based on access, affordability, insurance coverage, quality, and numerous social and identity factors, or the difficulties institutions face navigating reimbursement, insurance, and the pharmaceutical industry.
This hugely complex system of systems can feel like an insurmountable barrier to what seems like a simple task—providing care to the people who need it most, meeting them where they are in what are often some of the hardest times in their lives, and creating a supportive work environment for the staff who give so much of themselves to provide that care. Meanwhile, we need greater focus on preventative care and wellness to improve the overall health of our communities, and greater emphasis on across-the-board collaboration would result in reduced costs and improved care.
So how can architects help healthcare organizations successfully navigate and adapt in these challenging conditions? Our short answer: work within what we can control, focusing our experience and passion and bringing our problem-solving, consensus-building, and strategic-planning capabilities to the table. But let’s go deeper.
We talked with the BWBR healthcare principals, who are immersed in these issues and are deeply engaged with both executives and front-line staff in systems of varying sizes across the country. These wide-ranging discussions were incredibly enlightening, and revealed three specific, impactful ways design can support healthcare providers.
Create Exceptional Environments
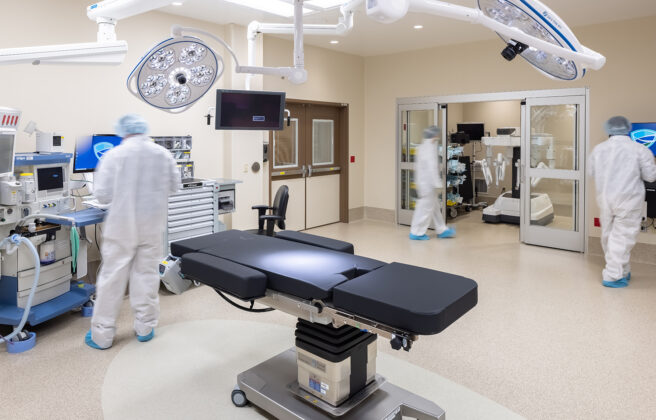
It’s likely no surprise that the first way architects and interior designers can have a tangible impact is by designing aesthetic spaces that work hard. For starters, this means bringing a hospitality mindset to the patient experience, looking for ways to make the entire journey flow smoothly, easing any friction points, and helping individuals and families navigate their care in a calming, welcoming, streamlined manner. We also apply the lens of the services being provided – for instance, extra care should be taken to provide daylight and views in an oncology clinic, where patients often spend hours at a time getting treatment.
That empathic approach extends to the staff experience as well. The people providing care are the true heart of the patient experience and, in the face of growing recruitment and retention challenges, addressing staff needs through outdoor access, places of respite, natural light, and collaborative spaces is crucial. Our discussions with staff underline the impact of addressing their physical and emotional needs, which can look like designing for a culture of safety while also optimizing for staffing levels and travel patterns to cut down on time spent walking versus caring for patients.
At the core of all of the above is a laser-focus on operational efficiency—we do this by asking the right questions of the right people, translating accurately between designer-speak and healthcare providers’ needs, and helping clients think outside the box by imagining new ways to work and share space so that both patients and staff can have the best possible experience.
Focus on Fiscal Responsibility
Also of utmost importance is the need to be cost-conscious, finding ways to deliver incredible design on budget. By centering the needs of the users, we keep the focus on function and purpose rather than on design for design’s sake. Our goal is always to serve as a trusted advisor to our clients, and that starts well before the design phase, as we work together to help understand your market, confirm we’re building within budget, right-sizing the facility to match your demand, and backing it all up with data. (For many projects, this begins with master planning, making sure to tie back to your organization’s strategic plan.)
Balance is the name of the game here, finding ways to deliver a beautiful space that speaks to your patient and staff needs without overdesigning or feeling institutional. We also work to keep costs low on our side, streamlining our workflow and budgeting as early as possible for transparency and flexibility. Our teams understand that there are many ways to create efficient flow and a welcoming environment without overspending and are committed to a collaborative process that does just that.
Be Good Stewards
While good stewardship is obviously financial, we believe it goes beyond money to include all resources, including human and environmental. As institutions inherently committed to doing good, we support that work by making sure your facility is as adaptable and future-proof as possible. If telehealth is increasingly important for a given patient population, the space must accommodate the privacy and technology needs that go along with that. This includes considering energy efficiency, operational resilience, ongoing maintenance, and operational optimization. We seek to pack increased function into reduced footprints, analyzing departmental adjacencies and opportunities to flex and share space.
Data is hugely important here too as a means of truth-testing assumptions. Rather than just jumping into a requested scope, we dig in with our clients to understand if the data backs it up, if there are other alternatives to be considered, and if the proposed approach is the best and highest use of resources before we start putting pen to paper. While these conversations are not always easy, they are worth having, and our team can offer an outside perspective to help you see things in a new light. A project does not have to result in construction for us to provide value or help you achieve your goals—and in some cases, not building might be the right move.
A Problem Shared
Experts estimate that clinical care and delivery contributes only about 20% to overall health outcomes; other contributors include individuals’ health behaviors, social and economic factors, and the physical environment. As a result, our clients must be focused on clinical care while also recognizing the importance of addressing other root causes of poor health, balancing an inward focus on the health system itself and an outward focus toward community-based interventions.
While it can be easy to feel discouraged in the face of such a complex web of systemic issues, economic pressures, and competing priorities, our team finds hope and direction by choosing to focus on innovating healthcare delivery while advocating for the people who deliver and receive care–that’s the honor and privilege of our work.